Thyroid And Anxiety
Contents:
- Hypothyroidism
- Hyperthyroidism
- Euthyroid Sick Syndrome
- Thyroid Storm
- Autoimmune Thyroiditis
- Graves’ Disease
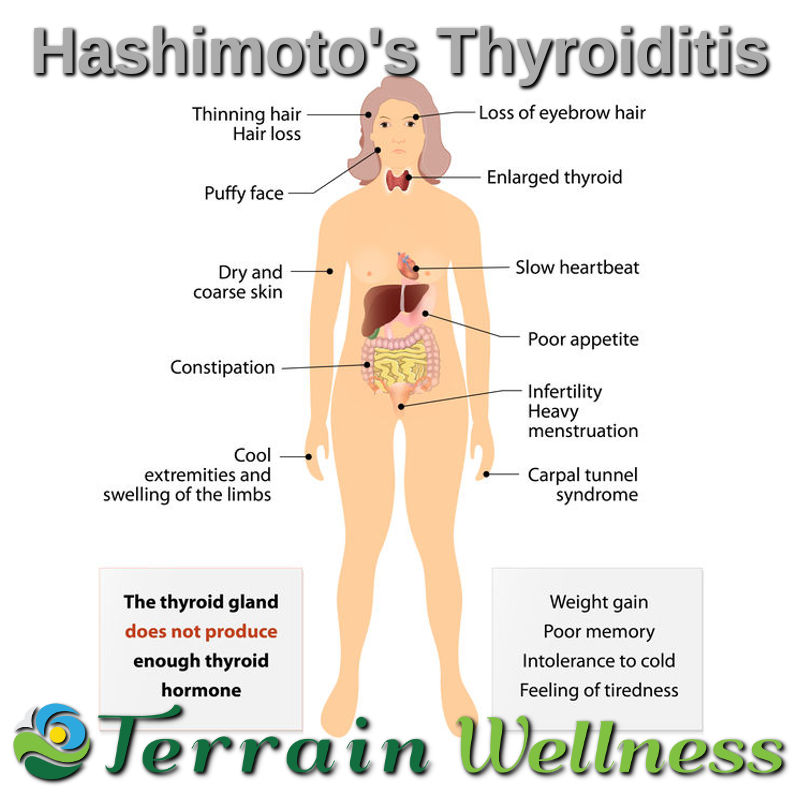
- Hashimoto’s Thyroiditis
- Autoimmune Thyroid Treatment
- Natural Thyroid And Anxiety Treatment
- Find The Right Doctor
Perhaps the most insidious thyroid symptoms are those that impinge upon our mood and emotions. With a direct impact on our relationships, careers and sense of well-being, the mood swings punctuated by angst and bouts of depression that define hormone imbalance can quickly destabilize our lives. Despite the frequency with which thyroid patients report feelings of anxiety and depression, these common symptoms are nonetheless frequently treated with psychiatric medications like anti-depressants or anti-anxiety pills, leaving their underlying thyroid imbalance untreated.
Too often, patients end up on medications like Synthroid and a benzodiazepine but their doctors do not take the extra time to deconstruct the underlying health and emotional conditions that led to the problem in the first place. Even more troubling is the fact that thyroid and anxiety problems can become a self-reinforcing pattern. Endocrine imbalance can amplify negative emotions, which in turn, can easily lead to unhealthy eating, poor sleep and foregoing self-care. This self-reinforcing pattern further disrupts our hormones.
So, how exactly are thyroid and anxiety or depression related? And, what are some simple steps that most people can take to start making a positive impact on their hormone balance, mood stability and sense of well-being? Since endocrine imbalances are complex cases, a doctor’s supervision is always recommended. That said, we’ll also discuss what to look for in a doctor. I strongly recommend finding a doctor with functional and natural medicine experience because those skills go beyond simply prescribing medications while instead guiding you toward sustainable, lasting health.
Euthyroid, Hypothyroid, Hyperthyroid
- Hypothyroidism

This is the most well-known condition and is defined by lower than normal T3/T4 levels in the body. This condition brings along all of the usual symptoms like fatigue, brain fog, gaining weight, feeling cold, loss of muscle strength, feeling cold and depression. Although this condition is commonly associated autoimmune conditions like Hashimoto’s Disease, other factors like chronic inflammation, long-term stress creating excess cortisol and food/lifestyle choices play a role in developing this condition.
- Hyperthyroidism

This is an adverse health condition where the body has too much T3/T4 hormones in the body. An excess of these very necessary hormones results in numerous body processes being put into an unhealthy overdrive state defined by symptoms like anxiety or irritability, fine muscle shakes in hands/fingers, weight loss, rapid or irregular heartbeat, enlarged/swollen thyroid (neck), reduced libido, sweating and heat sensitivity. Graves’ Disease is an autoimmune condition where the body attacks the thyroid due to often undiagnosed stressors like reactivated Epstein-Barr Virus, chronic inflammation, unhealthy gut bacteria among others. This is the most common reason why people develop hyperthyroidism (excess T3/T4), but there are other less common causes like eating too much iodine, goiter and certain types of thyroid lumps called nodules (specifically hot nodules).
- Clinical Euthyroid (Euthyroid Sick Syndrome)

Clinical Euthyroid, also called Euthyroid Sick Syndrome, nonthyroidal illness syndrome or just Euthyroid for short, is a medical condition where T3 hormone levels are low despite the gland appearing healthy and normal. The exact mechanism by which this condition develops is complex and not always readily apparent. That said, it appears that a buildup of Reverse-T3 (an inactive form of T3) and excessive pro-inflammatory cytokines are involved.
High levels of rT3 can be related to high Cortisol (a stress hormone), chronic inflammation, low iron levels and liver issues. Aside from surgery, severe injury or heart attack, reasons for a patient to present as clinically euthyroid may include excessive dieting, out-of-control stress, poor gut health and improper nutrition. Interestingly, a growing body of medical research indicates that anxiety, not depression, is more common in clinically euthyroid patients.
- Thyroid Storm

At times of particularly high stress or other provoking factors, hyperthyroidism can escalate into a medical emergency situation known as a Thyroid Storm. During a thyroid storm, anxiety may become severe to the point of great distress. Symptoms of this condition include racing heart rate (beating over 140 beats per minute), confusion, agitation, restlessness, shaking, sweating, diarrhea, confusion and losing consciousness. If you think you’re having a storm, call 911 and seek immediate emergency medical care.
Among thyroid disorders, there are three main conditions which may be present: clinical euthyroid (Euthyroid Sick Syndrome), hypothyroid and hyperthyroid. Autoimmune diseases like Hashimoto’s Thyroiditis may display different conditions as the body attempts to cope with underlying inflammation, poor gut health or reactivated EBV. The biology of hyperthyroid anxiety can be a little complicated, but the medical research shows that higher than normal T3/T4 results in significantly higher levels of adrenaline. While some adrenaline is helpful, too much is harmful to the body while also resulting in raised anxiety and elevated stress.
Progression of Autoimmune Thyroiditis
Early on, illness progression may exhibit symptoms of Graves’ Disease like anxiety or irritability, fine muscle shakes in hands/fingers, weight loss, rapid or irregular heartbeat, enlarged/swollen thyroid (neck), reduced libido, sweating and heat sensitivity. At this stage, the body’s immune system has begun attacking the thyroid gland’s TSH (Thyroid Stimulating Hormone) receptor site by creating antibodies called TRAb (TSH Receptor Antibodies). Medical research highlights the strong correlation between reactivated Epstein-Barr Virus and thyroid autoimmune conditions (see PubMed Study Here). When the body attacks its own TSH receptor site, it kicks production of T3/T4 into overdrive, resulting in a hyperthyroid condition.
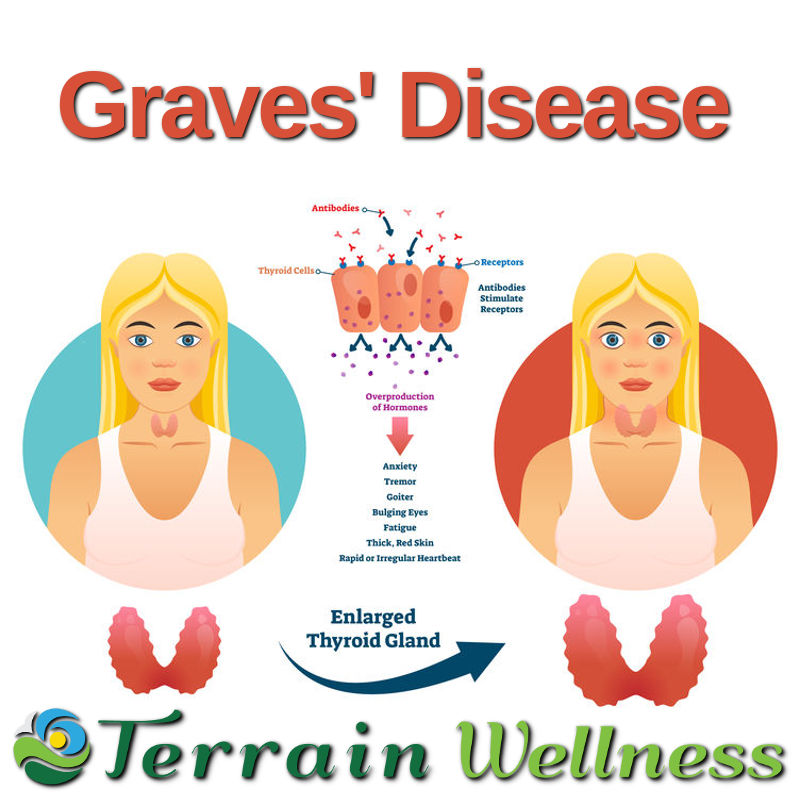
Unfortunately, the standard of care for Graves’ Disease often involves being prescribed anti-thyroid medications, surgically removing all/part of the gland or even radioactive iodine therapy to simply kill this important gland off over time. Anti-thyroid drugs suppress hormones in an effort to alleviate the over-production of T3/T4, but they don’t address the contributing factors that led to the autoimmune condition in the first place. Even more problematic is the use of radioactive iodine to speed up the killing off of the thyroid gland by directly aiding in its destruction. The problem with surgically removing a crucial part of one’s endocrine system is self-evident in that it makes one dependent on thyroid medications for life while doing nothing to dismantle the autoimmune process that created the problem to begin with.
If the thyroid hasn’t already been completely ruined by previous treatments for Graves’ Disease, the gland will become weaker from constant attack combined with producing hormones far beyond the healthy limit for a long time. When the gland begins to fail because it cannot keep up the excessive T3/T4 production demands and being continually attacked, patients generally shift from a hyperthyroid state to one of hypothyroidism.
Also see: thyroid hair loss.
At this point, Graves’ Disease transitions over to Hashimoto’s Disease (see: Graves’ Disease to Hashimoto’s). Symptoms at this point include weight gain, fatigue, feeling puffy and cold, pale skin, depression and joint/muscle pain. But, it doesn’t stop there. Once the immune system has wreaked havoc on our oh-so-important little butterfly-shaped gland in our necks, it moves on to cause further harm on other body systems. According to author and pharmacist Izabella Wentz, late-stage Hashimoto’s Disease can easily progress to other autoimmune conditions like Celiac Disease, Psoriasis, Rheumatoid Arthritis, Lupus, Multiple Sclerosis among others. Please note that this autoimmune progression occurs despite supplementing with Synthroid etc because hormone replacement does nothing to dismantle the dangerous underlying autoimmune process.
Functional, Natural Medicine Approach to Autoimmune
In contrast to the above, the natural/functional medicine approach to treating autoimmune conditions doesn’t stop at simply stabilizing the patient with hormone replacement or suppression. Rather, we seek to diagnose and alleviate the underlying factors that contribute to the development of these disease processes. The evidence shows that EBV and autoimmune thyroid conditions are clearly related. But, you don’t have to take my word for it (see PubMed: Graves’ Disease and EBV). My article on Epstein-Barr Virus treatment goes into more detail than I can here, but suffice it to say that in my clinical experience, as in the medical research, autoimmune thyroid conditions don’t usually “just happen for no reason”. By treating things like EBV, inflammation and gut health, we seek to dismantle the conditions that created the autoimmune response in the first place.
Natural Ways to Help Thyroid and Anxiety
While treating/managing autoimmune conditions that attack hormone-producing glands generally requires medical intervention, the foundation of good health has always been defined by the foods we eat, how we cope with stress and our lifestyle choices. Rebuilding that foundation to better support proper endocrine function goes a long way in improving quality of life and in some cases even reversing autoimmune conditions.
- Drop the Standard American Diet

The way most Americans eat has been linked to thyroid-harming inflammation, diabetes, heart disease, weight gain and cancer. Processed foods, refined carbohydrates and sugar encourage the overgrowth of unhealthy gut bacteria that cause inflammatory and autoimmune processes in the body. Additionally, the repeated blood-sugar spikes from too many refined carbs sets the stage for diabetes, which causes more thyroid problems.
- Get rid of “diet foods”

Diet foods seem too good to be true, and surprise, they generally are. Sugar substitutes have been found to evoke the same diabetes-inducing insulin spikes as real sugar because the body responds by trying to lower blood-sugar as if you had eaten real sugar resulting in a blood-sugar crash. In this way, calorie-free sweeteners are likely be worse for you than real sugar. Other so-called diet foods often have some aspect that may mislead people into thinking it’s a healthy food choice when it isn’t. Organic junk food is still junk food and gluten-free doesn’t automatically mean healthy (believe me, I wish it did). Watch out for foods like yogurt that may start out with beneficial properties like probiotics but end up so loaded down with carbs/sugar that they turn into junk food too.
The bottom line is that diet foods don’t really solve the problem of those jagged, thyroid-damaging blood-sugar booms and busts. Not only this, but imbalanced blood sugar results in feelings of nervousness, anxiety and irritability. As hard as it might be at first, ditch the diet foods.
- Choose Natural, Unprocessed Foods

Natural, unprocessed foods that are low on the Insulin Index offer sustained energy, more complete nutrition and freedom from endocrine-damaging (and anxiety-inducing) blood-sugar spikes. Not only that, but high-carb and processed foods are also tied to inflammatory and autoimmune processes in the body that can lead to hyperthyroidism in the short term, and Hashimoto’s in the long-term. Many patients have had success with aspects of Ketogenic, Mediterranean and Paleo meal plans. Although I don’t believe in one-size-fits-all nutrition, incorporate foods like avocado, spinach, kale, broccoli, nuts, whole eggs, fish (but beware of the mercury), chicken, turkey and some red meats for the iron.
- Avoid Excessive Dieting & Overtraining

Excessive dieting has been linked with anxiety in that it puts the body in a constant fight-or-flight response due to lack of food. The stress of dieting too much (often combined with overtraining) results in increased stress hormones while also depleting the body’s nutrients faster than they can be replaced. The production of hormones within the body requires minerals, fats and even the “bad” cholesterol. Diets that excessively limit calories, fats and cholesterol might work for a little while, but long-term these tactics can cause real harm to our endocrine balance.
I see many highly athletic patients with very “healthy” meal plans come into my office with symptoms of hormone imbalance like anxiety or depression. These patients have followed strict meal plans and often strict exercise programs for lengthy periods of time, but have begun to see their performance, fitness and health begin to slip. The problem is usually some mix of over training combined with an overly restricted meal plan. For example, most people who leave the Standard American Diet and go vegan quickly notice very real health improvements in the short-term. However, I also see many long-time vegans have their health begin to decline as things like B-Vitamin deficiencies, reactions to soy and continual blood-sugar spikes from often carb-heavy foods each take their toll.
Similarly, intense fitness routines over long periods of time can leave the body depleted of nutrients like Vitamin D, Iron, B Vitamins, Iron, Magnesium, Zinc and Omega III fatty acids. This is particularly extended-time cardio and training programs that don’t allow for adequate recovery. Ironically, over-training and excessive dieting can actually lead to increased stress hormones that hinder weight-loss and also decrease health and fitness over time. If you eat clean and work out a lot but you’ve noticed a decrease in athletic performance, mood, hormone balance, menstrual cycle or well-being, there’s a chance we need to evaluate your labs and custom-tailor a meal-plan that better meets your needs. Just as fitness evolves, so should your training, food choices.
- Natural Stress Reduction

As physicians, it’s sometimes tempting to view the human body from a purely physical perspective. However, this doesn’t tell the whole picture of the human experience. Our emotional health has a huge and ongoing impact on our physical well-being. Long-term or chronic stress is linked to heart disease, high blood pressure, stroke, weight gain, sexual dysfunction, digestive problems, hormone imbalance and death. Treatments like NET (Neuro-Emotional Technique), acupuncture and mindfulness are important aspects to my medical practice because our emotional health has such a huge impact on our physical health.
Unlike health conditions that can be looked at from a physical perspective, much of the human stress response lies in how we process (or avoid processing) our feelings and emotions. In my clinical experience, people’s health is tied to their emotional well-being, the quality of their relationships and how well they process stress. It may seem overly simplistic, but taking up mindfulness practices like meditation, deep breathing, yoga, time in nature or just simply getting in touch with one’s emotions can all help to reduce the toxic stress that can so easily creep into our lives. Most of us have blamed our stress on things like work, family, romantic relationships, children, our pasts or even traffic. Nonetheless, how we respond to all of those unpleasant circumstances is entirely up to us. Bad circumstances happen, but it is each of us who has the power to control the story that we place around those things.
Life can be hard and we learn 10 times as much about algebra growing up as we do about emotional well-being. However, learning healthy ways to decompress, let go of stress and reclaim the negative narratives that surround the circumstances of life pays us back in improving our health, our relationships and our experience of life.
Further Reading:
Does Your Doctor Understand Natural, Functional Medicine?

Consulting a doctor experienced in natural or functional medicine, thyroid health and endocrine balance is strongly recommended. As a doctor, I treat the patient in front of me, rather than just looking at a few basic lab tests. Too often, the medical establishment’s standard of care is to run a basic hormone test and prescribe a medication once things get bad enough. The main issue I have with the normal standard of care is that it does not intervene until the patient’s test results show a serious problem.
In contrast, there are small changes that we can make early on using naturopathic and functional medicine techniques so that more serious medical interventions like hormone replacement may be unnecessary. While I can and do write prescriptions, I do so sparingly. Overworked healthcare professionals who have to abide by increasingly stringent insurance guidelines may be cajoled into just writing a prescription and then moving onto the next patient. However, as a private membership practice, I keep working with patients toward the more sustainable, long-term goal that they reach a state of health where medications are no longer needed.
Thyroid conditions related to anxiety, depression and mood swings don’t just happen randomly. Knowing this, I work together with my patients to address underlying health conditions that contribute to imbalanced hormones. Nutrient deficiencies, estrogen dominance, an overgrowth of certain gut bacteria, imbalanced blood sugar, the Standard American Diet, stomach acid levels, heavy metals and long-term stress are just a few of the underlying health conditions that negatively affect the thyroid.
We also can’t fully treat thyroid and anxiety without looking at our emotional and spiritual well-being. When I treat patients for depression, anxiety and hormone imbalance, I’ve found adjunct treatments like acupuncture, meditation and Neuro Emotional Technique (NET) to be useful facets of integrative medical care. Neuro Emotional Technique is one of the methods I use with patients because it helps the limbic system (the part of the brain responsible for Fight or Flight responses) process and recover from past trauma. While NET, acupuncture and meditation practices are not “cures”, they can be used to down-regulate many of the biological systems related to long-term stress and anxiety.
While we are accepting new patients, no matter who you see as your doctor, make sure they’re willing to go beyond the normal lab panels because the standard tests are often too basic to diagnose these types of complex cases.
Conclusions:
Note that my general suggestions may not be right for everyone and there may be specific situations where a health condition contra-indicates generally sound advice. While my treatment protocol for endocrine imbalances is custom-tailored to each individual patients’ needs and lab test results, there are some common practices that patients can do at home that can often help improve their hormone health. Endocrine balance begins with food, lifestyle and how well we process and let go of emotional stress.
Yours in Health,

About the author:
I am an Oregon licensed primary care physician as well as a licensed acupuncturist. While my status as a Doctor does give me full prescriptive rights, I prefer to use more gentle, natural techniques when possible. I attended USC School of Dentistry for my undergraduate degree and the National University of Natural Medicine for my doctorate. My status as both a physician and an acupuncturist trained in classical Chinese medicine gives me a unique perspective on healthcare.